Punctal Plug Procedure: What to Expect Before, During, and After

You’ve been managing dry eye disease for a while now: the drops, the discomfort, maybe a prescription or two. And at your last appointment, your ophthalmologist mentioned punctal plugs as a possible next step.
The explanation was probably brief. A tiny plug, placed in the tear drain, to help keep moisture on the eye. It sounded simple enough in the office. But somewhere between leaving and getting home, the questions started:
A plug? Near my eye? What does that actually feel like? Will it hurt?
This article is a direct answer to those questions. Not the clinical summary — the honest, step-by-step walkthrough. What the doctor does, what you’ll feel in the chair, and what to expect in the hours and days after.
Table of Contents
What Happens Before the Appointment
For most patients, there is no separate procedure visit to schedule. In my practice, if we have already been managing your dry eye and plugs are the right next step, insertion happens the same day, adding about 30 seconds to the appointment.
If it is your first visit, or if plugs haven’t come up before, a full dry eye evaluation comes first. This means assessing whether your eyes produce enough tears, how quickly the tear film breaks down between blinks, and examining the surface of the eye, including the cornea and eyelid margins. The goal is to confirm that punctal occlusion is actually what your eyes need, because not all symptoms of dry eye have the same cause, and plugs work best when tear drainage is a meaningful part of the problem.
There are also situations where the right call is to wait, even when plugs are otherwise a good fit. Active infection, significant inflammation, or severe eyelid margin disease are reasons to hold off. Placing plugs while the surface is already irritated can make things worse rather than better. In those cases, the underlying issue gets addressed first, and plugs are revisited once the eye is in better shape.
When everything looks suitable, the visit itself requires no special preparation on your part. No fasting, no medication changes, nothing to arrange in advance. You can drive yourself to the appointment and resume your normal activities, including work, exercise, or screen time, immediately afterward.
Step-by-Step: How Punctal Plugs Are Inserted
Considered one of the most predictable minor procedures in ophthalmology, the insertion itself takes less than a minute, and it almost always surprises patients with how unremarkable it turns out to be.
You sit at the same exam chair used for any routine eye visit. The first thing I do is apply numbing drops, a topical anesthetic, directly to the punctum, the small opening at the corner of your eye that helps drain tears through the tear ducts. The drops work quickly, and from this point on, pain is simply not part of the experience.
Next, I gently pull the lower eyelid to expose the punctum and get a clear view of the opening. The lower puncta are almost always the starting point, and in the vast majority of cases, they are the only ones we need. The lower drainage opening accounts for roughly 75 to 80 percent of tear outflow, which means a single plug placed there is often enough to make a meaningful difference.
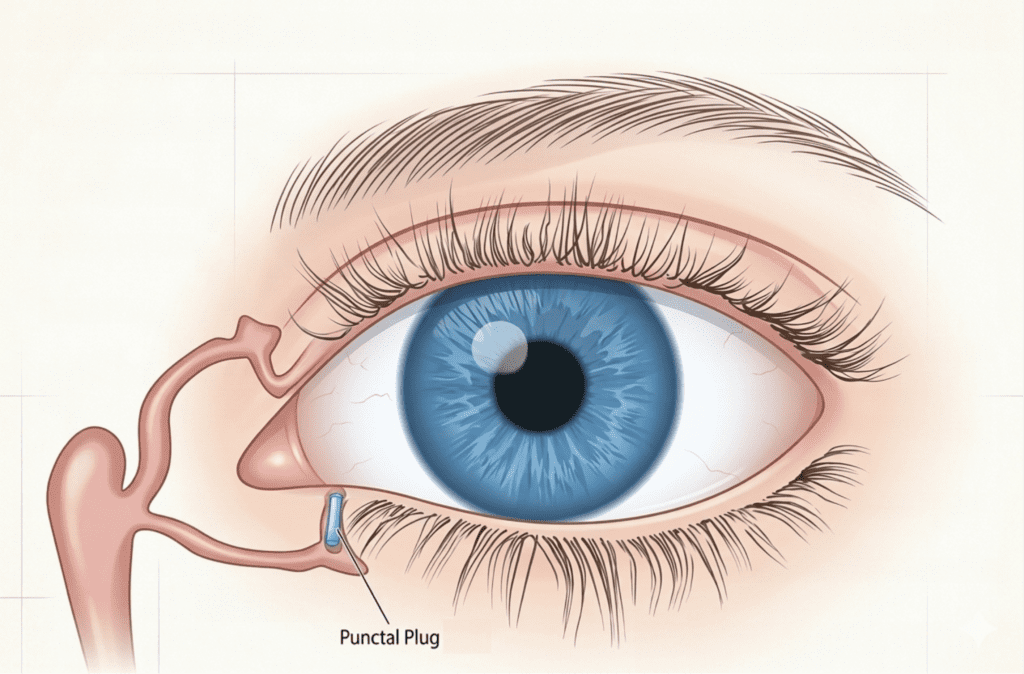
Upper plugs are only added in about 10 percent of cases, and only when lower plugs alone haven’t provided sufficient relief.
The two main types of punctal plugs are temporary collagen plugs and semi-permanent silicone plugs, sometimes also referred to collectively as lacrimal plugs or punctum plugs. They differ in both their design and insertion technique.
For collagen plugs, I use a small pair of non-toothed jeweler’s forceps to hold the plug during placement. Patients sometimes notice a brief moment of contact near the eye, but there is nothing sharp or pointed involved: the forceps grip the plug, not the tissue. The plug is then guided to the punctal opening and gently tapped into position. The right fit is one that slides in with a little resistance but doesn’t require force, snug enough to stay in place, not so tight that it’s uncomfortable. If the first size is slightly off, switching to the next size up or down takes only a few seconds.
For silicone punctal plugs, the technique differs slightly. These are semi-permanent plugs designed to remain in place longer than collagen. Rather than forceps, a pre-loaded inserter tool is used to dilate the punctal opening and release the plug into position. And unlike collagen plugs, which disappear entirely into the canal, silicone plugs have a round, flat cap, often described as mushroom- or umbrella-shaped, that remains visible at the surface of the eyelid once placed. This cap prevents the plug from migrating further into the drainage system and allows it to be removed with forceps if needed.
The visual confirmation at the end depends on which type was used. A correctly seated collagen plug should be fully inside the canal, with nothing protruding. With a silicone plug, the flat cap should be sitting flush at the punctal opening. Either way, a quick blink is the final check that the plug stays in position. At that point, the procedure is done.
What the Patient Actually Feels During Punctal Plug Insertion
The most common surprise patients report after punctal plug placement is how little they actually felt. The numbing eye drops applied before insertion are highly effective, and for most people, the experience is limited to a brief awareness of touch, nothing more.
When the eyelid is gently positioned and the plug is placed, patients typically notice a light sensation at the inner corner of the eye. Because the punctum sits on the eyelid rather than on the surface of your eyes itself, it does not feel like having something touch the eye directly. It is closer to a light press at the corner of the eyelid — momentary, and then gone.
Some patients feel almost nothing and are caught off guard when told the plug is already in. Others notice a short moment of pressure or awareness lasting only a second or two. The variability is normal and comes down largely to individual sensitivity and how much anticipation a patient brings into the chair. Anxiety, in particular, tends to heighten awareness, not because it makes the procedure more uncomfortable, but because it makes patients more attuned to every sensation.
Throughout the insertion, verbal guidance helps keep things calm and efficient. Patients may be asked to look in a specific direction, keep their eyes relaxed, or avoid squeezing their eyelids while the plug is placed. These simple cues keep the eyelid still and allow the plug to be positioned quickly and accurately.
For patients who are nervous going in, one of the most grounding things to hear is that this is a procedure many eye doctors have had done on themselves. I have collagen plugs placed in my own eyes — I deal with dry eye syndrome too, and they help reduce how much I rely on drops throughout the day. If this were uncomfortable or carried meaningful risk, it would not be something I would choose for myself.
When both eyes are being treated, the second plug almost always feels easier. The first placement sets the expectation; the second confirms it.
What to Expect After the Procedure
Immediately After
Once the plugs are in place, the appointment ends the same way a routine eye exam does. There is no recovery period and no waiting time in the office. Most patients simply stand up from the chair and continue with their day.
In the first few minutes after insertion, some people notice a mild awareness at the inner corner of the eyelid, a faint sense that something is there. This is normal and typically fades quickly as blinking returns to its usual rhythm. Most patients leave without any noticeable sensation at all.
The effect of the plugs themselves is gradual rather than immediate. By retaining natural tears on the surface of the eye, most patients begin to notice a subtle improvement in comfort within the first week. Not a dramatic shift, but a quiet reduction in the dryness and irritation they had been managing.
It is worth knowing what to watch for in the hours that follow. A sudden, intense foreign body sensation is the most common signal that a plug may have dislodged. This is not necessarily cause for alarm, but it is worth a quick visit to have the position checked. Redness, signs of infection, or any change in vision are also reasons to be seen, though these are uncommon with collagen plugs.
The First Days and Weeks
There is no real settling-in period with punctal plugs. For most patients, the days after insertion are uneventful. The plugs sit quietly in the tear drainage opening without being noticeable during normal blinking, and daily life continues without interruption.
Improvement tends to be gradual rather than immediate. Some people describe their eyes simply feeling less dry by the end of the day, or reaching for lubricating drops less often. The change is subtle at first and builds over the course of the first week or two.
It is also common for the two eyes to respond slightly differently, with one improving sooner, or symptoms fluctuating from day to day. This is normal, and the advice I give all my patients during this period is the same: don’t compare the two eyes, and try not to be hyper-focused on every sensation. Dry eye symptoms vary naturally, and over-monitoring tends to amplify awareness rather than help it.
Early Complications and How They’re Managed
With collagen plugs, true complications are rare. The most common issue is simply that a plug falls out, and patients may notice a return of their dryness symptoms or a brief foreign body sensation as it dislodges. If it falls onto the surface of the eye rather than out entirely, it can be easily removed at a follow-up visit. Replacement, if needed, is as straightforward as the original insertion.
The more significant complications associated with punctal plugs, including infection and internal migration, are largely specific to silicone plugs, which can become lodged deeper within the drainage system if they shift. Silicone plugs can also occasionally cause excessive tearing or watery eyes if the level of occlusion is greater than the eye needs. This is one of the main reasons collagen plugs are the preferred choice in this practice: the risk profile is simply much lower.
If a patient finds that they cannot tolerate the plugs, whether from persistent discomfort or a general sense that the eyes just do not feel right, that is a valid reason to remove them. Collagen plugs are temporary plugs that dissolve naturally over time, but they can also be taken out. The decision to stop is always straightforward, and there is no harm in trying and deciding they are not the right fit.
Follow-Up, Monitoring, and Next Decisions
Follow-up after punctal plug insertion is built into routine dry eye treatment rather than treated as a separate procedure visit. For collagen plugs, the natural check-in point is when the plugs are due to be replaced, typically a few months after insertion. If other treatment options are being introduced at the same time, or if there is active inflammation to monitor, we may schedule a visit sooner.
At that appointment, the conversation is straightforward: how has the dry eye been since the plugs were placed? Have symptoms improved? Is artificial tear use down? The surface of the eye is also examined to see whether the tear film looks more stable. These findings, taken together, give a clear picture of how much the plugs are contributing.
If the benefit has been meaningful, the plugs are replaced, and we continue. If the improvement is partial, other treatments are layered in, such as prescription drops for inflammation, or eyelid-focused treatments like IPL or radiofrequency to address gland dysfunction. The goal at every follow-up is to assess how well punctal plugs work within the broader treatment plan, and to make adjustments that support long-term eye health.
Special Contexts: Surgery, Eyelid Anatomy, and Patient Considerations
One setting where punctal plugs are particularly well-suited is around ocular surgery. Before LASIK or cataract procedures, collagen plugs help stabilize the tear film and improve the accuracy of pre-surgical measurements, and I place them routinely for this reason. This is especially relevant for patients who previously relied on contact lenses, as LASIK-associated dry eye can be significant. In the postoperative period, I like to keep them in place for roughly the first six months. The ocular surface is under real stress after surgery: the preservatives in post-operative drops can be irritating, and the cornea needs stable tear coverage to heal well and achieve its best vision. Retaining tears during this window makes a meaningful difference.
Eyelid anatomy is worth assessing before placement. If the lower lid is not sitting flush against the eye, an eye condition known as lid laxity, tear retention provides no meaningful benefit because the tears cannot spread across the surface properly. In those cases, there is no point in placing plugs until the eyelid issue has been addressed.
Patient sensitivity and history are also practical considerations. Some patients are genuinely reactive to touch around the eyelids, not simply nervous, but uncomfortable in a way that makes the procedure difficult to complete well. Patients who have had plugs before and found they did not work for them are unlikely to benefit from another attempt. In both situations, it is worth directing attention to other aspects of dry eye management rather than proceeding with insertion.
Older patients often present the opposite scenario. Dexterity limitations from arthritis or other conditions can make consistent drop use hard to maintain. For these patients, I particularly like placing punctal plugs. They provide steady support without requiring anything between visits, and that independence from frequent instillation makes a real practical difference.
Cost, Coverage, and What the Visit Looks Like
Insertion is performed in the exam chair during a regular dry eye appointment, with no separate procedure visit required. Placement adds only a minute or two to the overall visit. Follow-up works the same way: plug replacement and reassessment happen alongside routine dry eye care rather than as standalone appointments.
On the coverage side, it varies by plan. If a deductible is in place, that applies, but for most patients, the procedure is otherwise covered. Our front desk can help clarify what to expect for any individual plan before the appointment.
How to Prepare for a Punctal Plug Appointment
There is very little to do before a punctal plug appointment, and that is deliberate. The procedure is designed to add as little burden as possible to an already demanding condition. It is quick, performed in the exam chair with numbing drops, and requires nothing special in advance.
No fasting, no changes to regular medications, no need to arrange a driver. You can drive yourself to and from the visit and return to work, exercise, or screens immediately afterward. The goal is for the day to continue as normal.
Any questions about what to expect, including what the procedure will feel like, whether it is reversible, and what follow-up looks like, are best raised at the appointment itself. That conversation is part of the visit, and if anything gives you pause, there are always alternatives worth discussing.