LASIK Age and Suitability Guide: The Right Age for Laser Eye Surgery

If you are considering LASIK (laser-assisted in situ keratomileusis), one of the first questions that usually comes up is simple but loaded: am I too young, too old, or somewhere in the right window?
LASIK is one of the most common forms of laser vision correction and LASIK eye surgery for refractive errors such as nearsightedness, farsightedness, and astigmatism.
Because LASIK is an elective procedure that permanently reshapes the cornea, most people do not want to look back later and feel they did it too early, waited too long, or misunderstood what the surgery could and could not fix. However, age by itself does not decide whether you are a good candidate. What matters more is how age affects the parts of the eye surgeons actually evaluate: prescription stability, corneal health, tear film quality, lens changes, and your visual goals.
The real question is not how old you are or what the best age is, but whether your eyes are at the right stage for LASIK to be safe, effective, and worth it.
This article explains how age affects LASIK candidacy, why the timing question feels so stressful, what surgeons look for in younger and older patients, and when another procedure may make more sense than LASIK.
Table of Contents
How Age Actually Affects LASIK Candidacy
LASIK reshapes the cornea, which is the clear front surface of the eye. Age affects LASIK candidacy in a few main ways:
- Younger patients are more likely to still have changing prescriptions.
- Patients over 40 start dealing with presbyopia, which affects near vision.
- Older patients are more likely to have dry eye, often worsened by common medications.
- By the mid-to-late 50s, the natural lens may already be developing changes that make lens-based surgery a better long-term choice.
Age matters indirectly because it changes the likelihood of instability, dryness, presbyopia, and lens-related blur. Surgeons are not really screening for a birthday. They are screening for stability, safety, and whether LASIK matches what you want your vision to do.
Why Prescription Stability Matters Before LASIK
Prescription stability is the single most important age-related requirement that surgeons evaluate. While LASIK can correct your current vision prescription, it cannot prevent your eyes from continuing to change afterward. If the surgery is performed before the prescription has truly settled, you may see well for a while but still become nearsighted or otherwise dependent on eyeglasses again.
This is natural progression. It does not mean the LASIK surgery wore off.
This is the primary reason why surgeons want to see a prescription that is stable for at least a year. In many practices, the benchmark is less than 0.5 diopters of spherical equivalent change over 12 months, with a similar threshold for astigmatic change.
Some surgeons also look across a longer window, but the larger point is the same: if the numbers are still moving, the timing is probably wrong. Prescription stability is about making sure the surgery is likely to deliver effective, predictable, and lasting results.
A young eye that is still changing is harder to measure and treat accurately. Surgeons not only look for stable refraction, but they also need stable corneal measurements, including corneal topography and keratometry, with no signs of ectatic disease or a cornea that appears to be becoming more irregular over time.
This matters for two reasons. One is effectiveness: if the prescription is still changing, the result may not last as expected. The other is screening accuracy: if the eye has not fully stabilized, surgeons may be less confident that today’s measurements reflect where the eye is truly settling.
Hence, if the prescription is still moving, the recommendation is to wait until the measurements stabilize.
LASIK in Your Early 20s: When It May Be Too Soon
Early adulthood is the age range where many people are most tempted by LASIK and most likely to hear conflicting advice. Some are tired of glasses and contacts, while others want more freedom for work, travel, sports, or daily convenience. This is also the stage when prescriptions may still be drifting, especially in people with myopia.
The core issue with being “too young” is usually not age itself, but whether the eye has actually finished changing. If a surgeon recommends waiting, it is usually a sign they are protecting you from a result that may be less stable than you expect. Surgeons are careful about when to perform LASIK and whether it is actually likely to benefit the patient.
For patients in their early 20s, surgeons usually focus on a short set of readiness questions:
- Has the prescription been stable for at least 12 months?
- Is corneal mapping normal and symmetrical?
- Are there any signs the eye is still changing?
- Is the ocular surface healthy enough to get reliable measurements?
If the answer to those questions is yes, LASIK may still be reasonable in the early 20s. If not, waiting is often the better decision.
The FDA sets a minimum age of 18 for LASIK, but LASIK candidacy is not defined by age requirements alone. Most surgeons are looking for more than the minimum age. They want evidence that the eye has truly stabilized before doing a permanent procedure.
There are rare exceptions. In unusual medical situations, such as a patient facing meaningful harm from ongoing contact lens wear or someone with amblyopia (lazy eye) who cannot function well with standard correction, a surgeon may decide the balance of risk has changed. Those cases are exceptions, not the rule, but they show how surgeons really think: not in rigid age cutoffs, but in risk-benefit terms.
LASIK Between 25 and 40 Years: The Ideal Age Window
The age range from 25 to 40 is often considered the best LASIK window. By the mid-20s, most patients reach a stable prescription, corneal measurements are usually easier to trust, the tear film is often healthier than it will be later in life, and the natural lens is still clear and flexible.
In practical terms, this age range usually gives surgeons the most predictable combination of safety, accuracy, and long-term benefit.
However, everyone between 25 and 40 years is not automatically a candidate. Corneal thickness, topography, dry eye, pupil size, astigmatism, and general eye health still matter. But if someone has healthy eyes, good health overall, and a stable prescription, this range tends to offer the clearest and most durable distance-vision benefit from LASIK.
Patients often ask what long-term stability looks like if they have LASIK in their late 20s or 30s. In many cases, distance vision remains excellent for years, often until normal age-related lens changes later in life.
That is why surgeons often call this the ideal timing. The number itself is not magic. The eye is simply more likely to be in a stable and favorable stage.
LASIK in Your 40s and Early 50s: Managing Presbyopia
For people in their 40s and early 50s, the key question shifts to what vision problem LASIK is expected to solve. This is the decade when presbyopia starts to show up. Presbyopia is the normal age-related loss of near focusing ability caused by changes in the lens inside the eye. LASIK does not stop that process because LASIK works on the cornea, not the lens.
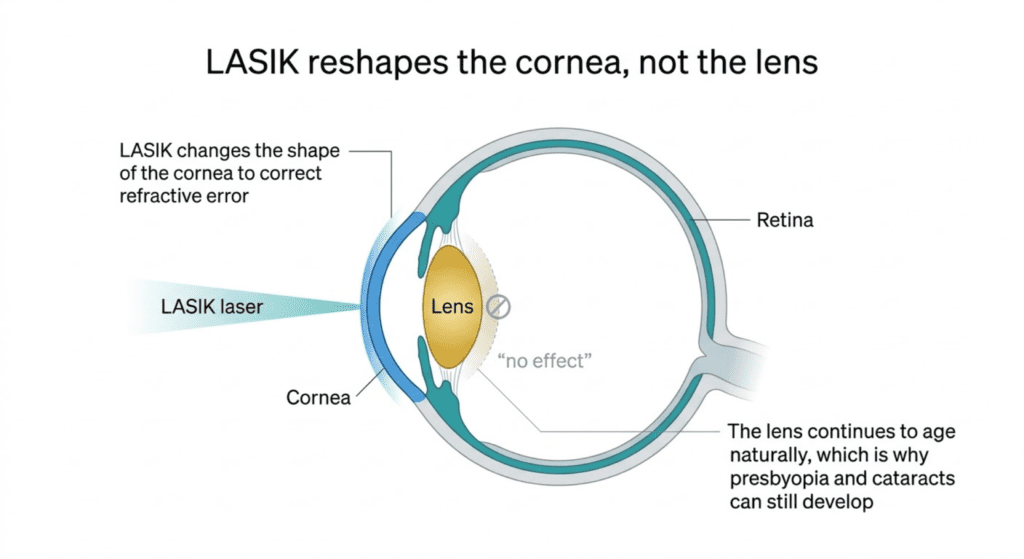
This is one of the biggest sources of confusion for patients. Someone may have excellent distance vision after LASIK, then need reading glasses later and assume the surgery failed. In reality, that usually means the LASIK worked and the lens aged exactly as expected.
One way to think about presbyopia is to imagine it as a wrinkle inside the eye. Over time, the lens and its supporting structures stiffen, so the eye loses the ability to shift focus up close the way it used to. That process happens whether you have LASIK or not.
That is why a standard distance-only LASIK plan can still work very well in your 40s, but only if you understand the tradeoff. You may love your distance vision and still need readers for close-up work.
For some patients, the better conversation is not just about LASIK, but about how to manage presbyopia realistically.
| Age Group | What Matters Most | Key Takeaway |
| Below 20 | Eye growth and prescription instability | LASIK is usually too early unless there is a rare medical reason to consider it. |
| 20 to 40 | Stable prescription, healthy cornea, good tear film | This is often the best LASIK window, provided the eyes are healthy and the measurements are stable. |
| Above 40 | Presbyopia, dry eye risk, and lens aging | LASIK may still work well, but the decision depends more on visual goals and whether a lens-based option makes more sense. |
Monovision and Blended Vision LASIK: When Surgeons Recommend It
Monovision LASIK is one of the main ways surgeons try to reduce reading-glasses dependence in patients with presbyopia. The idea is simple: one eye is targeted more for distance and the other is left slightly better for near tasks. The brain then learns to use each eye for different visual demands.
Monovision can work very well for the right patient, but it is not for everyone. Some people adapt easily. Others notice reduced depth perception, feel visually off-balance, or simply dislike the compromise.
That is why surgeons typically do not guess. They usually test eye dominance and use a contact lens trial before surgery to simulate what monovision will feel like in real life. Patients are often asked to go home, drive, read, work, and live normally with the trial lenses rather than judging them in a single office visit.
If someone does not tolerate the trial, surgeons generally do not proceed with monovision LASIK. In those cases, the plan may shift to standard LASIK plus reading glasses, or to a different type of refractive correction altogether.
LASIK After 55: When Lens-Based Surgery May Be a Better Option
There is no strict upper age limit for LASIK, but after 55 the decision often shifts from corneal correction to lens strategy. The real question is whether treating the cornea still makes sense when the lens is already aging.
Many patients in their mid-to-late 50s have at least early lens changes, even if they have not been diagnosed with a visually significant cataract yet. If the lens is starting to contribute to blur, glare, or fluctuating vision, LASIK will not fix the root problem because LASIK does not treat the lens.
This is why surgeons often bring up refractive lens exchange (RLE) or cataract surgery with premium intraocular lenses (IOLs) for older patients. Those procedures replace the aging natural lens and can address distance vision, near vision, astigmatism, and future cataract development in one plan.
This conversation can also be practical, not just medical. In the mid-to-late 50s, some patients already have early lens changes significant enough that insurance may cover part of a cataract-based procedure. That does not decide the treatment plan by itself, but it can make a lens-based option more realistic than patients expect.
All this does not mean LASIK is impossible after 55. Some patients are still appropriate candidates, especially if they have a clear lens, a healthy ocular surface, stable measurements, and a very specific goal such as distance correction only. But this is the age where many surgeons start with the lens conversation first, because it often becomes the more appropriate long-term option.
Eye Health Factors That Matter More Than Age
Several eye health factors matter more than age itself. Corneal shape is one of them. If topography suggests keratoconus or another unstable corneal pattern, LASIK may not be safe regardless of age.
Dry eye is another major factor. LASIK relies on accurate preoperative measurements and good healing afterward. If the tear film is unstable, the measurements can be unreliable and the recovery more uncomfortable. In some patients, dry eye treatment may need to be addressed before surgery.
Dry eye particularly becomes relevant with age because older adults are more likely to take medications that worsen dryness, including some blood pressure, hormonal, and psychiatric medications.
Pupil size and astigmatism also matter. Large pupils may raise the risk of glare and halos if more tissue has to be treated. High astigmatism may still be treatable, but it can affect which refractive procedure makes the most sense.
These issues do not necessarily rule out LASIK. They do change how carefully surgeons evaluate the eye and whether another procedure may offer better visual quality or a safer profile.
When LASIK Is Not Recommended at Any Age
Some reasons to avoid LASIK apply at any age.
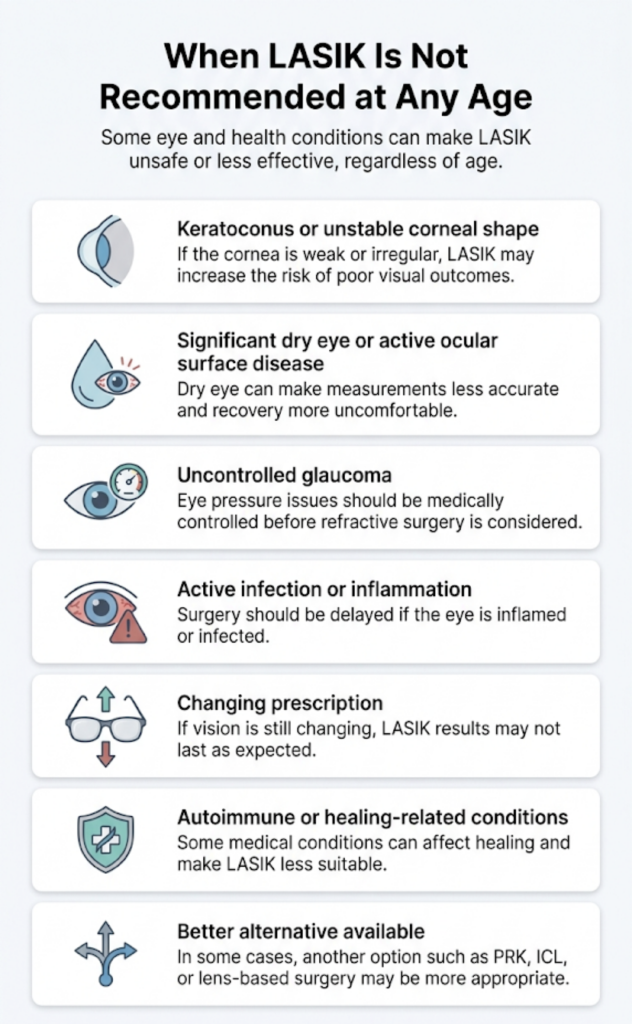
LASIK may not be recommended if you have:
- Keratoconus or a suspiciously unstable corneal shape
- Significant dry eye or active ocular surface disease
- Uncontrolled glaucoma
- Active inflammation or infection
- A prescription that is still changing
- Certain autoimmune or healing-related conditions
In those situations, the right conversation is not “How can we make LASIK happen anyway?” It is “What is the safest and most effective alternative?”
Good refractive surgeons do not force every patient toward LASIK. They match the procedure to the eye, the stage of life, and the patient’s real visual priorities.
How Surgeons Determine Your Personal Suitability
A LASIK consultation is not a yes-or-no screening. It is a decision-making process in which the surgeon assesses a number of factors, including:
- Refraction history to confirm prescription stability
- Corneal topography and tomography to study shape and symmetry
- Corneal thickness to estimate how much tissue can safely be treated
- Tear film and ocular surface health
- Pupil size and visual quality risk factors
- Lens clarity, especially in older patients
- Retinal health when relevant
Age changes how some of those findings are interpreted. For example, a mildly borderline corneal pattern in a 25-year-old may be more concerning than the same finding in a 45-year-old, because the younger eye has more time and more chance to continue changing.
That kind of judgment is where experience matters. The best consultations do not just ask, “Can we do LASIK?” They ask, “Is LASIK the best fit for this patient now, given where their eyes are and what they want their vision to be?”
Alternatives When LASIK Is Not the Best Option
If LASIK is not the right choice, refractive surgery may still be possible through a different procedure.
| Option | When It May Be Best |
| PRK | For patients who want corneal laser correction without a flap. |
| SMILE | For selected patients where the corneal profile and lifestyle make a flap-free option attractive. |
| EVO ICL | For higher prescriptions, strong visual-quality demands, or patients who are uncomfortable with the permanence of LASIK. |
| Refractive lens exchange | For patients whose real issue is no longer just the cornea, but the aging lens. |
| Cataract surgery | For patients who already have lens changes and may benefit more from lens-based correction than corneal surgery. |
The best alternative often depends on patient profile, not just the diagnosis.
Someone with a higher chance of being hit in the eye during sports, such as martial arts, may be steered toward PRK or SMILE because there is no flap, while a patient with a high prescription may be directed toward ICL to preserve corneal tissue and visual quality. A patient entering presbyopia may be better served by a lens-based solution.
A patient who is medically suitable for LASIK but emotionally stuck on the idea of irreversibility may feel more comfortable discussing EVO ICL because it is removable.
Setting Realistic Expectations About Age and Vision Correction
The most satisfied LASIK patients usually start with accurate expectations.
If you are in your early 20s, the key question is whether your eyes are truly stable. If you are in your 30s, the question is often whether this is the right time to enjoy years of glasses-free distance vision. If you are in your 40s, you need to understand that presbyopia is still coming. If you are in your late 50s or beyond, you need to know whether you are correcting the right part of the eye at all.
It also helps to know what LASIK does not do. It does not prevent presbyopia. It does not stop cataracts. It does not change the health of the retina or protect against other age-related eye disease. It corrects the cornea so your current refractive error is no longer dependent on glasses or contacts in the same way.
That may still be exactly the right solution. But it has to be the right solution for the stage of life you are in.
Making the Decision: Is This the Right Time for LASIK?
If you are worried about getting LASIK at the wrong age, you are usually asking the right question. That concern shows you are thinking beyond the sales pitch and focusing on timing, suitability, and long-term value.
For most people, the best answer is this:
- LASIK is often ideal from the mid-20s through the 30s if your prescription is stable and your eyes are healthy.
- LASIK can still work very well in your 40s and early 50s, but you need a clear plan for presbyopia.
- After 55, LASIK may still be possible, but lens-based procedures often make more sense.
If you are still feeling uncertain, it can help to compare LASIK not only with your ideal outcome, but also with the vision correction options you are using now.
For many long-term contact lens wearers, the alternative is not “doing nothing.” It is continuing a habit that can dry the eyes, reduce corneal oxygen exposure, and carry an ongoing risk of irritation or infection.
For patients who still cannot get comfortable with the permanence of LASIK, reversible options such as EVO ICL may be worth discussing.
So, what is the right age for LASIK? Usually, it is the age when your prescription is stable, your cornea is healthy, your lens is still the right target, and your expectations match what LASIK can realistically deliver.
That is why the best next step is not guessing based on age alone. It is getting a careful refractive evaluation and comprehensive eye exam from a surgeon who can tell you not just whether LASIK is possible, but whether it is the smartest choice for your eyes now.
Frequently Asked Questions About LASIK Age and Suitability
Does LASIK “wear off” over time?
No. The corneal reshaping is permanent. Later vision changes usually stem from natural aging of the eye’s internal lens, not a failure of the surgery itself.
Why must I wait until my 20s?
Surgeons require a stable prescription, typically less than 0.5 diopters of change over 12 months, to ensure the eye has finished growing before performing a permanent procedure.
Will I still need reading glasses after 40?
Likely. LASIK treats the cornea, but cannot stop presbyopia, the natural stiffening of the internal lens that makes near focusing more difficult with age.
Is LASIK safer than wearing contact lenses?
Often. Long-term contact lens use can cause infections or reduce oxygen exposure to the cornea. For healthy eyes, LASIK may be a safer medical outcome than decades of contact wear.
Am I too old for LASIK at 55?
Not strictly. However, lens-based procedures are often better at this stage because they address internal lens aging and cataracts, which LASIK cannot fix.